Tracheostomy
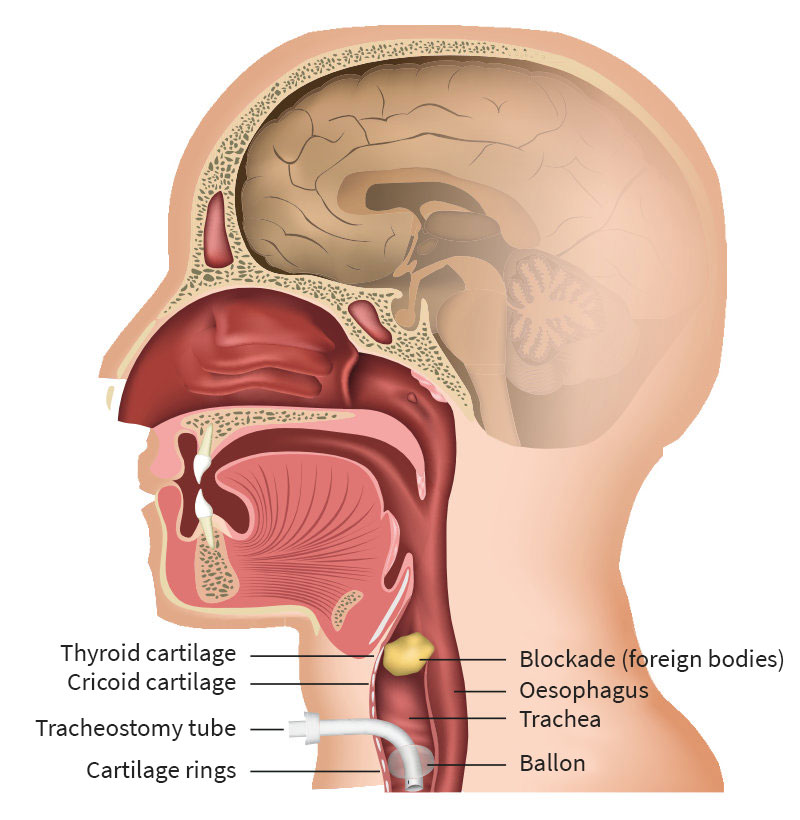
A tracheostomy is a frequently performed, very effective surgery to ventilate patients or in the event of a mechanical breathing disability in the larynx area.
A tracheostomy should not be confused with a cricothyrotomy which is performed in emergency situations on patients with an acute risk of suffocation.