Bronchial hyperreactivity
When we breathe, vital oxygen but also many irritants penetrate our lungs. Many people have a particularly sensitive reaction to such irritants – they suffer from bronchial hyperreactivity. What happens in the lungs of affected people and what can be done against it?
On a daily basis, our airways are continuously exposed to irritants that are present in the surrounding air. Exhaust fumes, cigarette smoke, pollen, dust, cleaners – to name just a few.
While most persons can easily tolerate these irritants, they can lead to symptoms from coughing and shortness of breath, all the way to serious choking attacks in persons with bronchial hyperreactivity.

Asthma and COPD as a common cause
Bronchial hyperreactivity denotes a hypersensitivity of the lungs. It appears most often, but not exclusively, in connection with allergies and pulmonary diseases such as bronchial asthma and COPD. If the triggering irritants penetrate the airways of these persons, they narrow the airways and may produce an urge to cough, feelings of tightness, and inability to breathe.
Triggers of obstructed airways
Triggers for bronchial hyperreactivity are primarily all of those irritants found in the air we breathe:
- Exhaust fumes
- Fine dust
- Cigarette smoke
- Cold air
- Perfume
- Cleaning chemicals
- Smoke
- Allergens such as pollen or dust mites
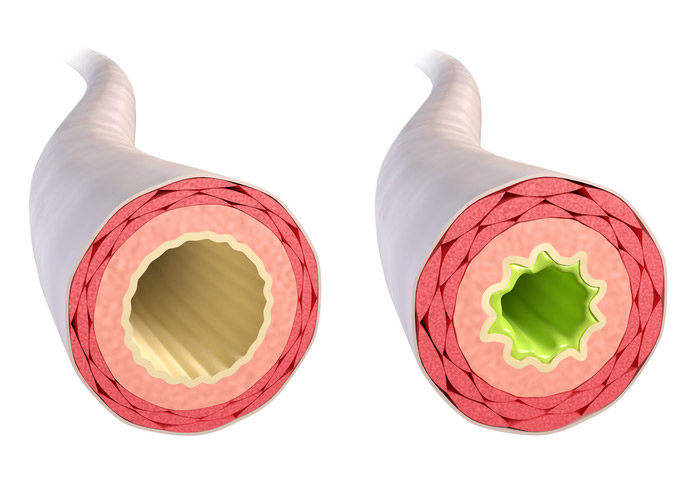
Symptoms of bronchial hyperreactivity
Generally, the symptoms of bronchial hyperreactivity (narrowed airways, coughing, shortness of breath) appear about 5 to 20 minutes after exposure, and disappear up to two hours later (immediate asthmatic response). In about 50% of cases, the symptoms reappear after 6 to 8 hours (late asthmatic response).
In certain weather situations, the symptoms often multiply: humid or wet weather also burden the airways and intensify the symptoms.
Furthermore, there are fluctuations in the bronchial hyperreactivity symptoms throughout the day, whereby symptoms become more pronounced in the evening and night hours.
Diagnosis of bronchial hyperreactivity
Bronchial hyperreactivity is diagnosed within the scope of testing, through the measurement of lung function (forced expiratory volume in 1 second, FEV1). Before such a measurement, any bronchodilating drugs that suppress narrowing of the airways must be suspended.
One simple method is measuring the lung function before and after an approximately 5-minute run. If the forced expiratory volume in 1 second drops by more than 15% after the endurance run, this would indicate bronchial hyperreactivity. Even a layperson can perform such a measurement using a lung function test for COPD.
Treatment of bronchial hyperreactivity
Treatment of bronchial hyperreactivity involves, to the extent possible, avoidance of the triggers. Early asthmatic responses are treated with bronchodilating drugs. In the case of late responses, they are mostly treated with inhaled corticosteroid sprays. In order to avoid side effects such as irritation of the vocal cords or fungus growth in the throat area, such sprays are administered using a spacer for inhalation (for example, the RC-Chamber®).
RC-Cornet® PLUS
RC-Cornet® PLUS NASAL
Subscribe to our
BREATHE EASY Newsletter
Tips and information on healthy airways!
- for all who wish to breathe better
- free of charge and convenient e-mails
- compact newsletter once a month
For all those who deal with pneumological topics related to the respiratory tract in a professional context, please find here the subscription to the CEGLA FACHNEWSLETTER.

